Shaky hands or sudden muscle spasms in seniors might be more than just aging. They can be signs of something as simple as, and as serious as, dehydration.
Plus, dehydration in seniors is often dismissed as a minor issue, but it can have far-reaching consequences, including on their nervous system. This article will help you understand the link between senior hydration and tremors and how to ensure your loved one stays safe and hydrated.
Your Loved Ones Need Good Care – Contact Us!
1. Why Older Adults Are Prone to Dehydration?
As we age, our bodies change in many ways that affect hydration. These changes make older adults vulnerable to dehydration, sometimes without even realizing it.
Staying hydrated is more than just drinking water. It’s about understanding the body’s needs and limitations.
Physiological Changes
Research proves that even though many seniors drink enough fluids most days, their bodies don’t always react well when extra hydration is needed. Factors like hot weather, being sick, or even light exercise can cause a fluid imbalance, plus older adults often don’t feel thirsty like younger people do.
As we age, our bodies adjust to having slightly thicker blood (called higher osmolality), so it takes longer to feel thirsty. On top of that, the sensors in our blood vessels, also called baroreceptors, that help signal when we need more fluids don’t work as well with age.
This means seniors may not realize they’re dehydrated until symptoms become more noticeable. Even after they start drinking water again, it may take their bodies longer to bounce back and fully restore fluid balance. That delay can lead to more serious issues if not addressed early.
Don’t Forget The Kidneys
A 2011 study also shows that as we age, our kidneys don’t work quite like they used to. For many seniors, these vital organs gradually lose their ability to filter blood as efficiently or hold on to fluids as they once did.
What’s going on behind the scenes? Well, several age-related changes in the kidneys make it harder for the body to stay balanced.
First, blood doesn’t move through the kidneys as quickly, and the tiny filters inside them, called glomeruli, start to wear out or become scarred. Some of these filters may even stop working completely. The kidneys can also shrink slightly and stiffen with age.
All of these changes add up to a slower and less effective system for managing hydration.
What Increases the Risk of Dehydration in Seniors?

Several common, everyday factors increase the likelihood of dehydration in older adults. Understanding these contributing factors allows caregivers and loved ones to take proactive steps.
- Medications: Diuretics, laxatives, antihistamines, and blood pressure medications can all lead to increased fluid loss. According to the Nutrients journal, these drugs are a primary contributor to dehydration in the elderly.
- Chronic Illnesses: Health conditions like diabetes, kidney disease, or heart failure can interfere with fluid balance. Some illnesses also come with side effects like vomiting or diarrhea, further contributing to dehydration.
- Mobility Issues: Seniors who have difficulty moving around may not get up to drink water regularly or may avoid it to reduce trips to the bathroom.
- Cognitive Decline: Seniors with dementia or Alzheimer’s may forget to drink water or be unable to communicate their thirst.
Recognizing Dehydration Symptoms in Older Adults
Early recognition is key to preventing complications. Caregivers should watch closely for these signs:
- Dry mouth and cracked lips
- Rough or dry skin
- Fatigue or unusual tiredness
- Dizziness or lightheadedness
- Dark-colored urine or low urine output
- Confusion, irritability, or sudden mood swings
- Headaches or blurred vision
Even mild dehydration can impact mental clarity and physical function in seniors, which is why it’s crucial to address it quickly.
2. How Dehydration Triggers Tremors
Tremors can be frightening, especially when they appear out of nowhere. While commonly associated with neurological disorders, tremors can also stem from something as correctable as dehydration.
Understanding the biological connection helps illuminate this scary symptom.
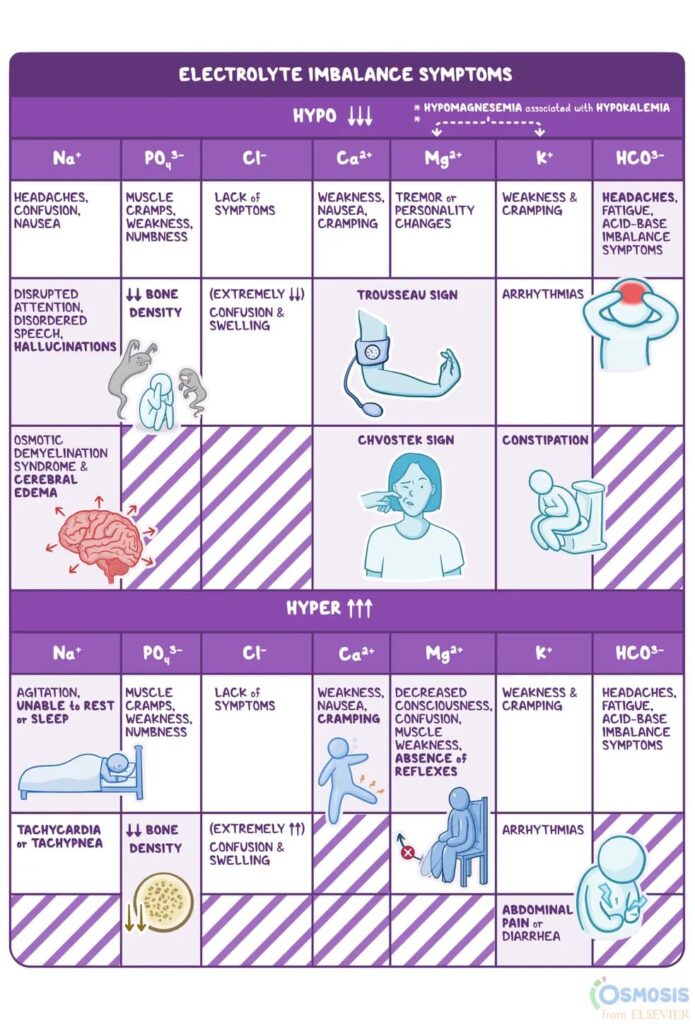
Electrolyte Imbalance and Tremors in Seniors
Our nerves rely on electrolytes, such as sodium, potassium, and magnesium, to function properly. These minerals help transmit electrical signals between the brain and peripheral nerves.
When someone becomes dehydrated, electrolyte levels can drop significantly. Research shows that even mild dehydration can alter electrolyte balance enough to disrupt nerve function and cause symptoms like tremors, weakness, or muscle twitching.
Disrupted Nerve Communication
Nerves need a well-hydrated environment to transmit clear signals. Without enough water, the balance of fluids inside and outside nerve cells becomes skewed. This impairs how nerves send and receive messages, leading to involuntary muscle movements or shakiness.
Muscle Cramping and Twitching
When muscles are deprived of hydration and essential nutrients, they can become overly sensitive and prone to sudden contractions. These can manifest as spasms or tremor-like symptoms.
Low levels of magnesium and potassium, common in dehydrated seniors, can lead to these types of muscle issues. Often, these symptoms worsen during physical activity or after prolonged sitting.
3. How to Identify Dehydration-Induced Tremors
Not all tremors are caused by dehydration. There are telltale signs that can help caregivers and nursing care distinguish between hydration-related symptoms and more serious medical conditions. Paying attention to context and symptom patterns is essential.
What Dehydration-Related Tremors Often Look Like
When dehydration is the cause, tremors typically:
- Come on Suddenly: Often after heat exposure, illness, or physical exertion
- Improve with Rehydration: Drinking water or electrolyte solutions can reduce or eliminate the tremors
- Lack a Neurological History: The senior has no previous diagnosis of neurological disorders like Parkinson’s or essential tremor
Dehydration-induced tremors in older adults are usually transient and less rhythmic than those caused by chronic conditions.
How It Differentiates from Other Conditions?
If tremors persist despite hydration or appear alongside other neurological symptoms, seek medical evaluation. Understanding the differences can help you or a loved one get the right care more quickly.
Essential Tremor
Essential tremor is one of the most common movement disorders. It typically affects both hands and occurs during voluntary actions, like writing, drinking from a cup, or tying shoelaces.
Unlike elderly dehydration tremors, essential tremors usually persist over time and don’t improve with rest or rehydration. They often run in families and may gradually worsen with age.
If a senior has had hand shaking for months or years, especially during activity, it might be this condition rather than a hydration issue.
Parkinson’s Disease
Parkinson’s disease is a progressive neurological disorder that comes with a unique set of symptoms, including:
- tremors at rest (not during movement)
- stiffness in the limbs
- slow movements
- and often a shuffling walk.
The tremors are more rhythmic and consistent when compared to those from dehydration. Also, Parkinson’s disease tremors usually do not go away with fluid intake, and symptoms gradually worsen over time.
If your loved one is also showing signs like slowness, muscle rigidity, or changes in facial expression, it’s worth discussing Parkinson’s disease with a doctor.
Medication-Induced Tremors
Some medications can lead to tremors as a side effect. These might include bronchodilators (often used for asthma), antidepressants, anti-seizure drugs, or even certain mood stabilizers.
If the tremors started after a new medication was introduced or the dosage changed, it’s worth reviewing the list with a healthcare provider.
Unlike dehydration tremors, which usually resolve with fluid replacement, medication-related tremors may persist until the medication is adjusted or changed. Always talk to a doctor before stopping or changing any prescribed treatment.
4. Prevention and Management

The good news is that dehydration is largely preventable. Whether in an assisted living or nursing home, caregivers can greatly reduce the risk of tremors and other complications. They can take a few simple steps and create hydration-friendly habits.
Your Loved Ones Need Good Care – Contact Us!
How Much Should Seniors Drink?
According to the National Council on Aging, most older adults should aim to drink at least 13 cups for men and 9 cups for women daily. However, individual needs may vary.
This includes water, decaf tea, low-sodium broth, milk, and foods with high water content like watermelon, cucumbers, or soup.
Here are a few helpful habits to support daily hydration
- Set Hydration Goals: Encourage seniors to drink a glass of water with every meal and snack.
- Make It Easy: Keep water bottles within reach in frequently used rooms.
- Offer Choices: Not everyone likes plain water. Herbal teas, flavored waters, or diluted fruit juice may be more appealing.
- Track Intake: Use a hydration log or app to track daily consumption.
- Use Cups with Lids and Straws: These are helpful for individuals with mobility or dexterity issues.
- Offer Drinks Frequently: This is important even if the senior doesn’t feel thirsty.
- Pair Fluid Intake with Routines: For example, encourage drinking after brushing teeth or before going to bed.
- Electrolyte-Rich Beverages: Consume drinks containing electrolytes, especially during illness or heat exposure.
- Balanced Diet: Ensure adequate intake of potassium, magnesium, and sodium through diet.
Addressing Special Situations
During illness, warm weather, or after exercise, fluid needs increase. Seniors who are vomiting, have diarrhea, or are on medications that cause fluid loss may need electrolyte-replenishing drinks.
Always consult a healthcare provider to ensure these are safe.
Regular Check-Ins Are Key
Routine wellness checks with a healthcare provider can identify early signs of dehydration. Medication reviews are incredibly important, as even new prescriptions can shift hydration needs.
Lastly, don’t hesitate to raise concerns about fluid intake at appointments.
Oral Rehydration and Severe Dehydration
For seniors experiencing mild to moderate dehydration, Oral Rehydration Solutions (ORS) can be a simple and effective way to replenish fluids and essential electrolytes. These solutions are readily available and easy to prepare, making them a practical option to combat dehydration at home.
However, in severe cases where dehydration cannot be managed through oral intake alone, medical professionals may need to administer intravenous (IV) fluids to restore hydration quickly and safely.
It’s important to seek professional advice to determine the best action based on individual needs.
5. When to Seek Medical Attention
Sometimes, symptoms go beyond what at-home hydration can fix. Knowing when to get help can prevent complications and keep your loved one safe.
Call a doctor or visit the ER if you notice:
- Tremors that do not resolve after rehydration
- No urine output for more than 12 hours
- Confusion, disorientation, or slurred speech
- Rapid heartbeat or shallow breathing
- Sunken eyes, cold extremities, or dry, wrinkled skin
- Loss of consciousness
These could be signs of severe dehydration, heatstroke, or another serious condition. When in doubt, it’s better to act quickly; timely intervention can save lives!
6. Role of Skilled Nursing Facilities

Skilled Nursing Facilities (SNFs) like Downey Community Health Center are vital in keeping seniors safe, especially when preventing and managing dehydration. With around-the-clock care and trained staff, SNFs are uniquely positioned to catch the early signs of dehydration and intervene before elderly dehydration tremors arise.
Your Loved Ones Need Good Care – Contact Us!
Here’s how facilities like ours support hydration every day:
24/7 Monitoring
At Downey Community Health, our nursing team is available day and night to keep a close eye on residents. This means we can catch signs of dehydration, like dry skin, confusion, or reduced urine output, early on. This is especially if the resident doesn’t mention feeling unwell.
Constant observation helps ensure that small issues don’t become major health concerns.
Assistance with Fluid Intake
We know that some residents may have difficulty drinking on their own, especially those with mobility challenges or cognitive conditions like a stroke.
Our staff gently encourages regular fluid intake and offers assistance as needed. This could mean holding a cup, using a straw, or simply reminding someone to take a sip.
We approach every resident with patience and compassion, treating hydration as a key part of overall care.
Regular Monitoring
Our care teams routinely check vital signs and assess hydration status during daily rounds. We pay attention to urine color, skin elasticity, and overall alertness.
If we notice anything off, we act quickly to increase fluid intake or involve a healthcare provider. These routine checks are a vital part of preventing dehydration before it becomes dangerous.
Through continuous care, personalized attention, and regular assessments, SNFs like Downey Community Health create a safer environment for seniors. One where hydration is not overlooked, and risks, like hydration-related tremors in the elderly, are actively managed.
Your Loved Ones Need Good Care – Contact Us!
Verdict: Dehydration is Fatal for Seniors, But Totally Preventable
Dehydration might seem like a simple issue, but in seniors, it has the potential to cause serious and confusing symptoms like tremors. The good news is that many of these effects are preventable with thoughtful care and consistent hydration.
As caregivers, being proactive and compassionate can go a long way. Watching for signs, building habits, and knowing when to seek help ensure our loved ones live safely and comfortably.